Health Library
Childhood Pancreatic Cancer Treatment (PDQ®): Treatment - Patient Information [NCI]
General Information About Childhood Pancreatic Cancer
Pancreatic cancer is a disease in which malignant (cancer) cells form in the tissues of the pancreas.
The pancreas is a gland about 6 inches long that is shaped like a thin pear lying on its side. The wider end of the pancreas is called the head, the middle section is called the body, and the narrow end is called the tail. The pancreas lies between the stomach and the spine.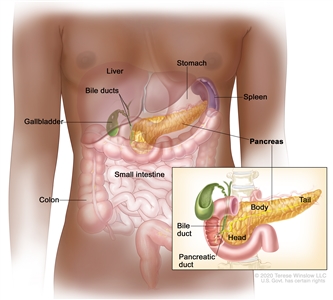
Anatomy of the pancreas. The pancreas has three parts: the head, the body, and the tail. It is found in the abdomen near the stomach, intestines, and other organs.
There are two kinds of cells in the pancreas:
- Endocrine pancreas cells make hormones, such as insulin and glucagon, that help control blood sugar levels. Both of these hormones help the body use and store the energy it gets from food. Endocrine pancreas cells cluster together in many small groups (islets) throughout the pancreas. Endocrine pancreas cells are also called islet cells or islets of Langerhans.
- Exocrine pancreas cells make enzymes that are released into the small intestine to help the body digest food. Most of the pancreas is made of ducts and small sacs at the end of the ducts that are lined with exocrine cells.
There are four types of pancreatic cancer in children.
The four types of pancreatic cancer in children include the following:
- Solid pseudopapillary tumor of the pancreas. This is the most common type of pancreatic tumor in children. It most commonly affects females that are older adolescents and young adults. These slow-growing tumors have both cyst -like and solid parts. Solid pseudopapillary tumor of the pancreas is unlikely to spread to other parts of the body and the prognosis is very good. Occasionally, the tumor may spread to the liver, lung, or lymph nodes.
- Pancreatoblastoma. It usually occurs in children aged 10 years or younger. Children with Beckwith-Wiedemann syndrome and familial adenomatous polyposis (FAP) syndrome have an increased risk of developing pancreatoblastoma. These slow-growing tumors often make the tumor marker alpha-fetoprotein. These tumors may also make adrenocorticotropic hormone (ACTH) and antidiuretic hormone (ADH). Pancreatoblastoma may spread to the liver, lung, or lymph nodes. The prognosis for children with pancreatoblastoma is good.
- Islet cell tumors. These tumors are not common in children and can be benign or malignant. Islet cell tumors may occur in children with multiple endocrine neoplasia type 1 (MEN1) syndrome. (See the PDQ summary on Childhood Multiple Endocrine Neoplasia [MEN] Syndromes Treatment for more information.) The most common types of islet cell tumors are insulinomas and gastrinomas. Other types of islet cell tumors are ACTHoma and VIPoma. These tumors may make hormones, such as insulin, gastrin, ACTH, or ADH. When too much of a hormone is made, signs and symptoms of disease occur. These tumors are also called pancreatic neuroendocrine tumors (pancreatic NETs).
- Pancreatic carcinoma. Pancreatic carcinoma is very rare in children. The two types of pancreatic carcinoma are acinar cell carcinoma and ductal adenocarcinoma.
Signs and symptoms of pancreatic cancer include feeling tired and weight loss.
General signs and symptoms of pancreatic cancer may include the following:
- Feeling tired.
- Weight loss for no known reason.
- Loss of appetite.
- Stomach discomfort.
- Lump in the abdomen.
In children, some pancreatic tumors do not secrete hormones and there are no signs and symptoms of disease. This makes it hard to diagnose pancreatic cancer early.
Pancreatic tumors that do secrete hormones may cause signs and symptoms. The signs and symptoms depend on the type of hormone being made.
If the tumor secretes insulin, signs and symptoms that may occur include the following:
- Low blood sugar. This can cause blurred vision, headache, and feeling lightheaded, tired, weak, shaky, nervous, irritable, sweaty, confused, or hungry.
- Changes in behavior.
- Seizures.
- Coma.
If the tumor secretes gastrin, signs and symptoms that may occur include the following:
- Stomach ulcers that keep coming back.
- Pain in the abdomen, which may spread to the back. The pain may come and go and it may go away after taking an antacid.
- The flow of stomach contents back into the esophagus (gastroesophageal reflux).
- Diarrhea.
Signs and symptoms caused by tumors that make other types of hormones, such as ACTH or ADH, may include the following:
- Watery diarrhea.
- Dehydration (feeling thirsty, making less urine, dry skin and mouth, headaches, dizziness, or feeling tired).
- Low sodium (salt) level in the blood (confusion, sleepiness, muscle weakness, and seizures).
- Weight loss or gain for no known reason.
- Round face and thin arms and legs.
- Feeling very tired and weak.
- High blood pressure.
- Purple or pink stretch marks on the skin.
Check with your child's doctor if you see any of these problems in your child. Other conditions that are not pancreatic cancer may cause these same signs and symptoms.
Tests that examine the pancreas are used to help diagnose pancreatic cancer.
The following tests and procedures may be used:
- Physical exam and health history: An exam of the body to check general signs of health, including checking for signs of disease, such as lumps or anything else that seems unusual. A history of the patient's health habits and past illnesses and treatments will also be taken.
- Chest x-ray: An x-ray of the organs and bones inside the chest. An x-ray is a type of energy beam that can go through the body and onto film, making a picture of areas inside the body.
- CT scan (CAT scan): A procedure that makes a series of detailed pictures of areas inside the body, such as the chest and abdomen, taken from different angles. The pictures are made by a computer linked to an x-ray machine. A dye may be injected into a vein or swallowed to help the organs or tissues show up more clearly. This procedure is also called computed tomography, computerized tomography, or computerized axial tomography.
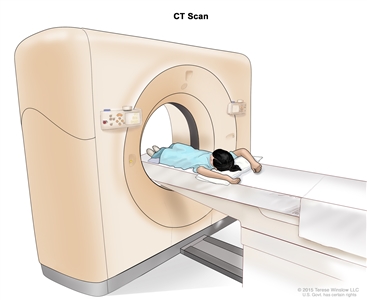
Computed tomography (CT) scan. The child lies on a table that slides through the CT scanner, which takes a series of detailed x-ray pictures of areas inside the body. - MRI (magnetic resonance imaging): A procedure that uses a magnet, radio waves, and a computer to make a series of detailed pictures of areas inside the body, such as the chest and abdomen. This procedure is also called nuclear magnetic resonance imaging (NMRI).
- PET scan (positron emission tomography scan): A procedure to find malignant tumor cells in the body. A small amount of radioactive glucose (sugar) is injected into a vein. The PET scanner rotates around the body and makes a picture of where glucose is being used in the body. Malignant tumor cells show up brighter in the picture because they are more active and take up more glucose than normal cells do.
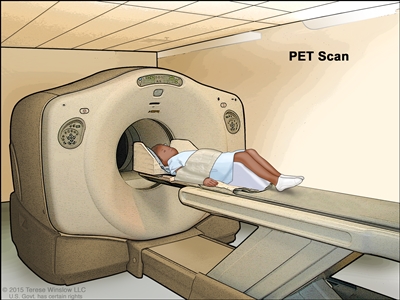
Positron emission tomography (PET) scan. The child lies on a table that slides through the PET scanner. The head rest and white strap help the child lie still. A small amount of radioactive glucose (sugar) is injected into the child's vein, and a scanner makes a picture of where the glucose is being used in the body. Cancer cells show up brighter in the picture because they take up more glucose than normal cells do. - Endoscopic ultrasound (EUS): A procedure in which an endoscope is inserted into the body, usually through the mouth or rectum. An endoscope is a thin, tube-like instrument with a light and a lens for viewing. A probe at the end of the endoscope is used to bounce high-energy sound waves (ultrasound) off internal tissues or organs and make echoes. The echoes form a picture of body tissues called a sonogram. This procedure is also called endosonography.
- Somatostatin receptor scintigraphy: A type of radionuclide scan used to find pancreatic tumors. A very small amount of radioactive octreotide (a hormone that attaches to carcinoid tumors) is injected into a vein and travels through the bloodstream. The radioactive octreotide attaches to the tumor and a special camera that detects radioactivity is used to show where the tumors are in the body. This procedure is used to diagnose islet cell tumors.
- Biopsy: The removal of cells or tissues so they can be viewed under a microscope by a pathologist to check for signs of cancer. Procedures used to obtain a tissue sample include the following:
- Core-needle biopsy: A procedure to remove tissue using a wide needle.
- Laparoscopy: A surgical procedure to look at the organs inside the abdomen to check for signs of disease. Small incisions (cuts) are made in the wall of the abdomen and a laparoscope (a thin, lighted tube) is inserted into one of the incisions. Other instruments may be inserted through the same or other incisions to perform procedures such as taking tissue samples.
- Laparotomy: A surgical procedure in which an incision (cut) is made in the wall of the abdomen to check the inside of the abdomen for signs of disease. The size of the incision depends on the reason the laparotomy is being done. Sometimes tissue samples are taken.



